In 1987, four years after the discovery of HIV as the causative agent of AIDS, scientists reported the first drug effective against the virus, called zidovudine. Zidovudine targeted a viral enzyme called reverse transcriptase, and prevented the virus from completing its life-cycle. However, zidovudine was no magic bullet. It could hold the virus at bay for a while, but HIV quickly learned to outsmart it, and the resulting drug resistance meant many patients soon lost the drug’s protective effect.
It quickly became clear why zidovudine alone would not keep HIV in check. The virus is exceptionally good at making copying ‘mistakes’ when it turns its RNA into DNA, generating endless new variants. Some of these variants possess the property of drug resistance. Importantly however, these changes can’t happen just anywhere. Some parts of the virus are so essential to its survival that they must remain largely unchanged. Altering them would break the virus itself.
So researchers decided to aim more drugs at these ‘must keep’ regions, where the virus has little room to evolve. The insight led to the development of multiple antiretroviral drugs targeting different viral proteins, including reverse transcriptase, protease, and integrase, laying the foundation for combination therapies that could suppress the virus far more effectively and durably.
Provocative question
In 1999, a paper in the journal Science detailed how another protein of HIV, called the capsid, folds into its unique protective shape. The study was important because the capsid is a structure that protects the virus’s RNA from the environment. The work provided the breakthrough to understanding how the capsid folds into its unique 3D structure. Soon, the same team reported that most mutations in the capsid protein could render HIV incapable of infecting cells, showing that it was much more vulnerable than previously believed.
The discovery raised a provocative question: if the capsid was so essential, and so fragile, could it itself be a drug target? For years, the answer seemed to be ‘no’. Scientists at major pharmaceutical companies started working on potential molecules that could latch onto the capsid and disrupt its carefully balanced structure, effectively stopping the virus in its tracks.
While one candidate seemed promising, it had a persistent problem: it didn’t easily dissolve in water. Since solubility was a basic requirement for most medicines to circulate reliably in the body, the researchers had to keep tweaking it to see if they could improve its solubility while maintaining its potency. Then, after more than two decades of persistence, the problem was turned on its head.
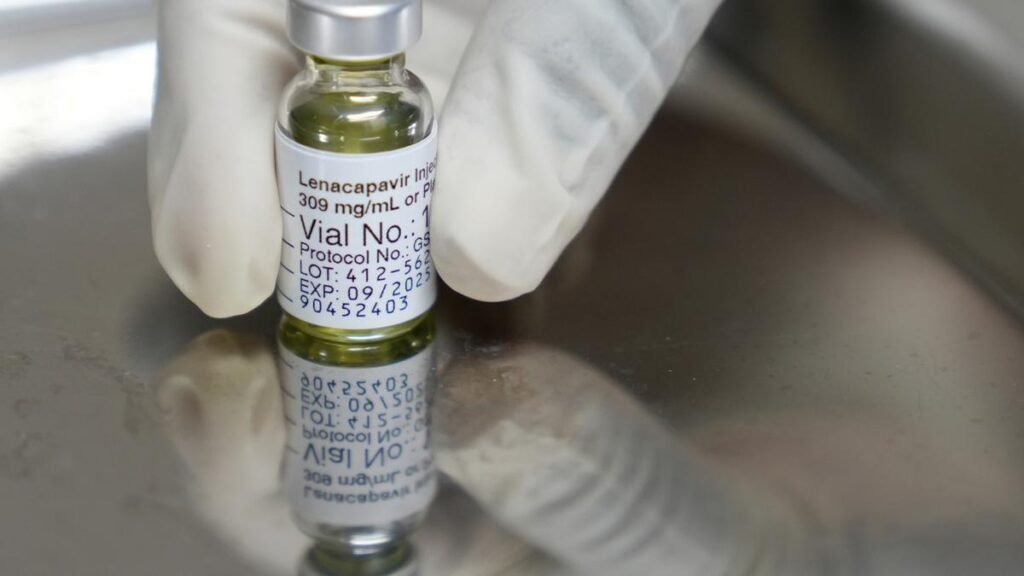
On June 18, 2025, the U.S. Food and Drug Administration (FDA) approved lenacapavir, the world’s first capsid-based HIV inhibitor. Its poor solubility, once a liability, became its greatest strength. Instead of being taken daily, lenacapavir is injected under the skin of the abdomen just once every six months, forming a slow-release reservoir that steadily delivers the drug into the bloodstream.
The results were astonishing: in clinical trials, it prevented HIV infection in high-risk individuals with 100% effectiveness. Lenacapavir was not a cure but, as a Science article put it, it may be the next best thing to an HIV vaccine.
Acting solo
However, one hard-learnt lesson from four decades of HIV research is that no single drug has ever escaped resistance. Given enough time, the virus finds a way, which is why HIV is always treated with combinations of drugs and never one alone.
In a study published recently in Science Translational Medicine, researchers from across the U.S., including the pharmaceutical company Gilead Sciences, examined viruses from patients who received lenacapavir as part of treatment, rather than prevention, and identified a small set of changes in the capsid protein, most commonly involving positions known that reduced the drug’s effectiveness.
Importantly, these resistance mutations emerged primarily when lenacapavir was acting alone, without other fully active drugs in the regimen. When lenacapavir was used in proper combination therapy, viral suppression was largely maintained, reinforcing the long-standing rule of HIV treatment: that the virus can escape one blockade but not many at once.
To test whether the resistance came at a price, the researchers engineered the drug-resistant viruses in the laboratory. They took capsid sequences from patients who had developed resistance, inserted those exact mutations into a standard laboratory HIV strain, then watched how these altered viruses behaved.
The results were striking. Viruses carrying the strongest resistance mutations often replicated at less than 20-30% of normal levels, even in the absence of the drug. In effect, escaping lenacapavir meant HIV had to damage one of its own components, the capsid, and that was the cost of its survival.
Shells of other viruses
The study reaffirmed the longstanding belief that the viral capsid is actually a very good drug target and that the virus can’t afford to change it too much. This certainty opens the door to a new generation of drugs that target the capsid, with the reassurance that resistance will come at a high cost to the virus. With this proof in hand, researchers can now explore capsid-focused strategies more aggressively, combining them with existing therapies.
Beyond HIV, the work also adds to proof that it’s a good idea for researchers to examine the protective shells of other viruses, which may be similarly vulnerable.
The four-plus decades of HIV research are a reminder that scientific progress is often slow, uneven, and unglamorous. For years, capsid inhibitors were under scrutiny and may have even been abandoned permanently if not for those researchers who kept at it, unwilling to abandon an idea they believed the science supported. If the story of lenacapavir teaches us anything, it is that sometimes, breakthroughs are the result of persistence and not inspiration.
Arun Panchapakesan is an assistant professor at the Y.R. Gaitonde Centre for AIDS Research and Education, Chennai.
Published – February 25, 2026 05:30 am IST